Print Entire Issue
Join us at the 8th Annual

KeePosted Info
Features
Medication Synchronization
Pharmacy Legislative Day 2014
Columns
President's Message
Directly Speaking
The GAS from Springfield
ICHPeople
New Practitioners Network
College Connections
Indian Health Services: A Unique Pharmacy Rotation in Ambulatory Care
Patient Care Projects to Promote American Pharmacists Month
More
Officers and Board of Directors
Welcome New Members!
ICHP Pharmacy Action Fund (PAC) Contributors
Upcoming Events
KeePosted Info
 Illinois Council of Health-System Pharmacists
Illinois Council of Health-System Pharmacists
4055 North Perryville Road
Loves Park, IL 61111-8653
Phone: (815) 227-9292
Fax: (815) 227-9294
www.ichpnet.org
KeePosted
Official Newsjournal of the Illinois Council of Health-System Pharmacists
EDITOR
Jacob Gettig
ASSISTANT EDITOR
Jennifer Phillips
MANAGING EDITOR
Scott Meyers
ASSISTANT MANAGING EDITOR
Trish Wegner
DESIGN EDITOR
Amanda Wolff
ICHP Staff
EXECUTIVE VICE PRESIDENT
Scott Meyers
VICE PRESIDENT - PROFESSIONAL SERVICES
Trish Wegner
DIRECTOR OF OPERATIONS
Maggie Allen
INFORMATION SYSTEMS MANAGER
Heidi Sunday
CUSTOMER SERVICE AND
PHARMACY TECH TOPICS™ SPECIALIST
Jo Ann Haley
ACCOUNTANT
Jan Mark
COMMUNICATIONS MANAGER
Amanda Wolff
LEGISLATIVE CONSULTANT
Jim Owen
ICHP Mission Statement
Advancing Excellence in the Practice of Pharmacy
ICHP Vision Statement
ICHP dedicates itself to achieving a vision of pharmacy practice where:
- Pharmacists are universally recognized as health care professionals and essential providers of health care services.
- Patients are aware of the training, skills, and abilities of a pharmacist and the fundamental role that pharmacists play in optimizing medication therapy.
- Formally educated, appropriately trained, and PTCB certified pharmacy technicians manage the medication distribution process with appropriate pharmacist oversight.
- Pharmacists improve patient care and medication safety through the development of effective public policies by interacting and collaborating with patients, other health care professionals and their respective professional societies, government agencies, employers and other concerned parties.
- Evidence-based practices are used to achieve safe and effective medication therapies.
- There are an adequate number of qualified pharmacy leaders within the pharmacy profession.
- Pharmacists take primary responsibility for educating pharmacy technicians, pharmacy students, pharmacist peers, other health professionals, and patients about appropriate medication use.
KeePosted Vision
As an integral publication of the Illinois Council of Health-System Pharmacists, the KeePosted newsjournal will reflect its mission and goals. In conjunction with those goals, KeePosted will provide timely information that meets the changing professional and personal needs of Illinois pharmacists and technicians, and maintain high publication standards.
KeePosted is an official publication of, and is copyrighted by, the Illinois Council of Health-System Pharmacists (ICHP). KeePosted is published 10 times a year. ICHP members received KeePosted as a member benefit. All articles published herein represent the opinions of the authors and do not reflect the policy of the ICHP or the authors’ institutions unless specified. Advertising inquiries can be directed to ICHP office at the address listed above. Image disclaimer: The image used in the Pharmacy Tech Topics advertisement is the property of © 2014 Thinkstock, a division of Getty Images.
Copyright © 2014, Illinois Council of Health-System Pharmacists. All rights reserved.
Features
Medication Synchronization
by Phil Burgess, RPh, Chairperson, Illinois State Board of Pharmacy
There have been numerous studies recently published that promote the utilization by pharmacists of “medication synchronization” for their patients in order to improve patient care. The basic concept is for pharmacists to coordinate the dispensing of patients’ medications (through obtaining refill approvals and making quantity adjustments) so that a schedule can be established for the patient to receive their multiple medications at the same time and even potentially on the same day of the month.
In a study published this July in the American Journal of Health-System Pharmacy (AJHP), a program implemented by Thrifty White Pharmacy in Minnesota demonstrated significant positive results by synchronizing the filling of prescriptions for a patient’s chronic conditions so that all of the medications are ready for pickup by appointment once a month. The article indicates that Thrifty White had almost 27,000 patients enrolled in the program in 91 stores for this “appointment based model” (ABM).
The results were impressive. The ABM patients were 3.4 – 6.1 times as likely as control patients (who were not part of the program) to be adherent to their prescribed regimen for the different medications. In this same AJHP article, it was mentioned that the Pharmacy Quality Alliance would be supporting the expansion of this model in hundreds of sites nationally.1
The Illinois Pharmacy Practice Act (85/20) states: “Nothing in this Section shall prohibit a pharmacist who is exercising his or her professional judgment from dispensing additional quantities of medication up to the total number of dosage units authorized by the prescriber on the original prescription and any refills.” By this act, within professional judgment, Illinois pharmacists have the flexibility to assist their patients in synchronizing the dispensing of their medications.
I am well aware that this whole program represents some third-party “challenges” due to day supply/quantity limitations. However, through a concentrated effort over the course of a few months, this can be accomplished. The end result will be improved patient care through better adherence to therapy. In my professional opinion, the most significant benefit will be the improvement in the patient counseling experience. When you are interacting with a patient and reviewing all of the medications at the same time…WOW! How different is that than what happens today?!
In today’s “high volume” environment, how realistic is this for all of your patients. It’s not. But start with just a couple of your patients with multiple disease states and medications. Work with their third party program if possible. If they are not cooperative, gradually move these patients towards having their refills all at the same time. You might want to do an internet search for “medication synchronization” to see how others have addressed this “challenge”. This is a tremendous opportunity to demonstrate your value as a pharmacist.
And as always…….Make Patient Care Your Priority.
Reference
1. Traynor K. Synchronized Prescription Fills Improve Patients' Medication Adherence. American Society of Health-System Pharmacists.
http://www.ashp.org/menu/News/PharmacyNews/NewsArticle.aspx?id=3920 (accessed 2013 December).
Pharmacy Legislative Day 2014
 Join hundreds of pharmacy professionals at the State Capitol on March 5, 2014!
Join hundreds of pharmacy professionals at the State Capitol on March 5, 2014!
Represent your profession and speak directly to legislators and staff regarding the critical
issues facing pharmacy. It is vital that your legislators become more knowledgeable on the role of pharmacy in augmenting healthcare.
Learn about key issues and how to discuss them with your legislators. Join your fellow pharmacists, students & techs and become part of the solution. Don’t miss this opportunity to let your collective voices be heard!
Jointly sponsored by Illinois Council of Health-System Pharmacists and the Illinois Pharmacists Association. For the past seven years, ICHP and IPhA have joined forces to let lawmakers know that pharmacists stand united.
You MUST be pre-registered to attend 2014 Pharmacy Legislative Day!
Registration Deadline: February 24, 2014
For more information or to register online or print a paper registration form, please
click here.
Columns
 President's Message
President's Message
Practice Based Learning
by Mike Fotis, ICHP President
You have probably worked with or served as a preceptor for pharmacy students and recent grads who completed courses in pharmacy school that followed a Practice Based Learning (PBL) teaching strategy. If you are a PGY-1 or PGY-2 resident preceptor who has completed Residency Learning System (RLS) training, you have likely been at least introduced to this concept. Many of the medical students and recent medical graduates that you interact with every day were taught using PBL methods. It is very likely that your kids, and for a few of us, your grandchildren are being taught by this method right now!
Once we entered college most of us were taught by the traditional lecture based strategy. In a four credit hour course, 3 one hour lectures were supplemented by a one hour discussion session led by a graduate student. The professor presented material in an organized and often (but not often enough) interesting manner. The grad students answered our questions, and led discussions that often helped us apply the information to structured situations. Attending a lecture is an effective way to gather facts, but students end up in a passive rather than active mode, and if you now serve as faculty or as a preceptor, you might have noticed that students might not remember these facts for very long after the final exam. As a preceptor I can attest that fact-based learning doesn't help very much with application and analysis skills, doesn't promote working as a part of a team, and doesn't help to develop the learning skills needed to be successful in experiential training.
For the past couple of years I have had the opportunity to serve as a tutor for Clinical Medicine using PBL methods. This year I also have PBL experience for parts of Pharmacology and for Medical Decision Making courses. In PBL the responsibility for learning rests squarely on the student. Each week in Clinical Medicine, an unstructured real life clinical case serves as the basis for our three weekly discussions. There are also lectures that help to introduce the material needed to address the patient case. In the first PBL session, students interview a virtual patient to gather data, formulate a problem and generate hypotheses. A virtual exam is conducted in the second session and the students use this information to rank and test hypotheses while later in the week lab tests and imaging are used to re-rank hypotheses. In the third session, hypotheses undergo further testing, and if an intervention is needed, a treatment plan is developed which may or may not include medications.
As you might expect, since the material is new to the students there are numerous issues that require further study. The students determine whether or not there is a “learning issue” (LI) and each student presents a summary of the learning issues at the next class. The students are dependent on each other to prepare a timely, thorough, and well referenced learning issue at each PBL class session. In the first year of this experience I was also serving as a preceptor for pharmacy students and often found myself pointing out in discussion with the pharmacy students that I thought the students had an LI and asked which of them were going to take responsibility for the LI. The pharmacy students looked at me in amazement wondering if having an LI was a healthy or unhealthy diagnosis! Believe it or not, the pharmacy students tended to like working in this manner (once I explained an LI was a Learning Issue), so I tended to use a modified PBL technique quite often.
It’s not easy serving as a PBL tutor, especially for me. As the teacher, you need to keep your mouth shut much more frequently than I am used to doing. It is best to let the students work together to solve the patient case, even though as an instructor, I am sorely tempted to help them. Many times you need to provide hints, but even though I had completed some formal and experiential PBL training provided by the University, I found that my hints alternated from too obvious, giving away the answer, to so obscure the students had no idea what I was talking about. Last year I was better at providing hints, and this year I think I have it figured out. The trickiest scenario is when the students have overlooked an important issue, or have misunderstood the physiology, pharmacology or have misunderstood Evidence Based Medicine. Asking the students to discuss the further implications of their hypothesis usually leads to recognition that they are on the wrong path. Don’t forget to use this method once in a while when the students are correct.
Another advantage of the PBL method is that students are better prepared for their clerkship experiences as many of the methods used in PBL are the methods used during their experiential education. Students take responsibility for their own learning, learn to work in groups and to trust one another, and I really appreciate when they develop a questioning and critical approach to the presented material. Most importantly, students are highly engaged in their coursework, take responsibility for their virtual patient, avoid simply memorizing material and instead develop their own understanding of each topic rather than repeating the instructor’s statements. I also want to point out that all of our students tend to prefer the PBL method.
Is PBL a panacea that will automatically solve all of our educational issues? Of course not. But even though I had always considered myself to be an excellent lecturer, I am so glad I had the additional opportunity to learn to use the PBL method. If your team has a tendency to focus on facts and tasks and might be missing the overall picture, you might want to learn more about the PBL strategy. If you or any of your residents would like to see PBL methods in action, please contact me. I would love to have the opportunity to have you on campus for a couple of classes.
 Directly Speaking
Directly Speaking
Change in Pharmacy Practice: Does It Just Happen or Can It Be Planned?
by Scott A. Meyers, Executive Vice President
First a confession – the title of this article is part of the title to a session at the recent ASHP Midyear Clinical Meeting. The full title of the session was “Change in Pharmacy Practice: Does It Just Happen or Can It Be Planned? Lessons from the Mirror to Hospital Pharmacy,” and it was moderated by one of health-system pharmacy’s most prominent visionaries, Bill Zellmer. The program obviously made an impression on me because I’ve chosen its theme, and part of its title for my January column.
The session featured Dr. Gregory Higby, Executive Director for the American Institute of the History of Pharmacy at the University of Wisconsin, and Douglas Scheckelhoff, Vice President for Professional Development for the American Society of Health-System Pharmacists as invited speakers. Dr. Higby presented a historical recap of the first survey of Hospital Pharmacy in the US which collected data from 1957-1963 and resulted in the publication of The Mirror to Hospital Pharmacy in 1964. The audit team responsible for the survey included Donald and Gloria Franke and Cliff Laitiolais, all well-known leaders in hospital pharmacy’s early days! The team started with two separate surveys, a larger 73-question survey sent to hospitals over 100 beds and a smaller 16-question survey sent to smaller hospitals (those under 100 beds). The results of those surveys can be found along with the entire free online “Mirror” here. The historical value of that publication is immense, and while its applicability to today’s health-system pharmacy practice is minimal, it is worth a read by anyone who wants to view the origins of today’s practice.
Doug Scheckelhoff reported on ASHP’s recent and current efforts to measure today’s practice in US hospitals and health-systems. In addition he made some valuable comparisons between practice circa 1960 and today. Most pharmacy directors in the 60’s weren’t interested in preparing sterile intravenous solutions much less could they imagine dealing with the requirements of USP 797 today. Doug’s slides are currently still available on the ASHP Midyear Clinical Meeting Website.
Bill Zellmer added his usual valuable insights and then brought forward two more practitioners to react to the presentations and respond to questions from the audience. Jim Stevenson, Director of Pharmacy at the University of Michigan and Joseph Bonkowski, Pharmacy Systems Manager at Wake Forest Baptist Medical Center, both provided their perspectives on what pharmacy’s future could be. Overall it was an outstanding program that I had just happened to find rather than a program I seriously planned to attend to give me more perspective on today’s pharmacy practice – interestingly similar to the title of the program!
But the real message I want to bring to you, the members of ICHP and the leaders of hospital and health-system pharmacy in Illinois, is that the future of practice often just happens but could be so much more if it were more frequently planned! Planning at the department level, thinking out of the box and further out than just reacting to problems as they surface will help departments move forward to better serve the patients it cares for and the institutions it serves. Searching our practice’s horizon and continuously scanning the local, state and national environment will help pharmacy personnel identify opportunities and arising problems early on so that changes can be made in a systematic and efficient method.
That’s easy to say when resources and time are not an issue. But ICHP can help. We will provide you with education and information that does more than provide solutions to today’s problems. We will continue to strive for educational excellence and professional programming and articles to help our members stay ahead of the curve. We will provide opportunities for pharmacy directors and clinical specialists to meet and share their problems and plans through the pharmacy directors’ network and clinical practitioners and research networks regular meetings. KeePosted will continue to provide valuable articles to keep you informed about changes in the practice act and rules, articles on medication safety and much more.
And we will look to you as you identify new opportunities or solve arising problems, to share what you have learned and done with your professional colleagues and perhaps future friends. We will continue to look to our members to help us move forward as we work on our mission of “Advancing excellence in the practice of pharmacy!” In 2014 we begin to update our strategic plan to better meet our members’ needs. We’ll ask you what you would like to receive as member benefits from us in the future in an effort to keep you and ICHP out on the cutting edge of practice.
ICHP will begin 2014 in a planning mode to work to improve practice. I hope you will begin a planning process no matter how limited or fundamental for your department. Begin a planning process that is proactive, to whatever extent you can afford in time and resources, in order to be more structured on how practice progresses in your institution. And if you already have an extensive planning process in place, let me know. I would love to learn about what you’re doing and perhaps your colleagues would, too. Practice change will continue to just happen in many cases, but let’s see if we can make more changes happen because we planned in 2014 than we have in the past. Happy New Year!
The GAS from Springfield
Tech-Check-Tech, no rules just right?
by Jim Owen and Scott Meyers
Well, the best laid plans of mice and men often fail to produce the desired results, and this is the case for the proposed rules on Tech-Check-Tech! After the second draft of the rules were sent out to the pharmacy organizations in Illinois, Tech-Check-Tech was a reality! But the reality of actual rules lasted for but a few weeks, and then they disappeared. Thanks to an objection by another pharmacy association who feared that rules written in Section 1330.530 On-site Institutional Pharmacy Services would be pirated and abused by the big chains, the Tech-Check-Tech rules have been removed completely from the draft that went to the Governor’s office for final review before publication in the Illinois Register. Unfortunately, they didn’t talk with ICHP first, or they may have seen that their complaint may have facilitated the exact action they most feared.
So what does that mean? We asked the Illinois Department of Financial and Professional Regulation that very question and their response was, “You can still use techs to check other techs work, it’s just that there won’t be any specific rules to govern the practice. The pharmacist in charge will be responsible.” This sounds well and good, but what happens if there is an administration change following the next Governor election (November of this year)? All bets could be off without specific rules on the books. Or more importantly, by not having these rules in the specific “On-site Institutional Pharmacy Services” section, the rules could be expanded to be used by the chains to fulfill that association’s biggest fear!
Unfortunately, this isn’t the only section of rules that went by the wayside after the second draft was distributed. Another pharmacy association had issues with the Medication Therapy Management rules that better described the pharmacist’s role under standing orders, and the result is that those clarifying rules have been removed, too. The concerns raised were in regard to two simple statements that read:
D) A standing order may not include the following:
1. Authority for the pharmacist to prescribe.
2. Authority for the pharmacist to diagnose.
The same draft rules included language that allowed the pharmacist to initiate, modify and discontinue medications. So our question is “what’s the problem?” Pharmacists are not trained to diagnose, so we have no beef there. And if the pharmacist may initiate, modify and discontinue medications per standing order, who really cares if the same rule says the pharmacist may not prescribe? But obviously someone felt differently. Will this stop pharmacists from asking physicians for standing orders to help manage their patients’ drug therapy? Probably not – but it will probably deter some pharmacists who prefer to have rules in black and white to guide their practices.
This demonstrates that communication between pharmacy organizations is critical at all times. Communications must be proactive and look for the common ground to seek a mutually beneficial solution! No one pharmacy association should try to speak for the profession because no one pharmacy association represents the entire profession! We need to work together, reach a shared solution and then go to the Department or in other cases the legislature with one response.
The real goal for pharmacy in the future should be, “If it’s not specifically prohibited, then we should be able to do it!” I know that sounds risky and easy to say for someone who has not been in direct patient care for many years, but it’s probably time for pharmacy to “Just do it!” rather than ask for permission and black and white guidelines to be put in place first.
ICHP will keep working with our friends in the other associations and try to convince them to talk to us before talking to the government. But we encourage you pioneers to go out and implement programs that you know will improve patient care and safety as long as you know they are not specifically prohibited by the Act or the Rules. It’s time to “Just do it!”
ICHPeople
 ICHP's very own Vice-President of Professional Services, Trish Wegner, was featured in ASHP's December 2013 Spotlight! Check it out!
ICHP's very own Vice-President of Professional Services, Trish Wegner, was featured in ASHP's December 2013 Spotlight! Check it out!
New Practitioners Network
Interprofessional Education – Finding Collaboration in Unexpected Places
by Rebecca Castner, PharmD, Assistant Professor of Pharmacy Practice at Chicago State University COP/Clinical Pharmacy Specialist, Ambulatory Care at Rush University Medical Center
As we know, and have all probably felt, the push for a more integrated educational model among pharmacy and other health disciplines seems to be growing stronger by the minute. However, unless we are part of the small number of educators who formally teach within an integrated, multidisciplinary curriculum, we may struggle with finding ways to regularly implement interprofessional education into our own practice. While this task may seem daunting, it may not need to be – as long as we’re ready to get a little creative. In this article, I will give a brief summary of how one of our community campus events at Chicago State University allowed us to integrate educational experiences among multiple disciplines, as well as give some insight that will hopefully help you find opportunities in unique places within your own practice.
Many of us are regularly involved in community events, which are prime opportunities to hold health fairs, and faculty at Chicago State University College of Pharmacy are no exception. Each year, CSU invites the surrounding community to its campus for a free jazz concert series called “Jazz in the Grazz,” and the pharmacy school has organized various health fairs at these events. However, instead of inviting other disciplines to participate and requesting they set up their own booth and activities independently, our pharmacy team instead requested the other disciplines join us in our activities to work alongside each other during two concerts this year, lending their own expertise to each station. These disciplines included nursing, pharmacy, occupational therapy, and health information administration. We invited all disciplines to a training/review session for the booths to be included in this health fair prior to the events, which also helped break the ice and begin communication among the students of various disciplines. Each discipline was distributed as equally as possible to form well-rounded interdisciplinary classes within the training.
To measure the impact of integrating the disciplines on the students’ education, we conducted a survey of students’ perceptions of their competencies in various areas before and after involvement in the events, based on the core competencies published by the Interprofessional Education Collaborative Expert Panel. Results of the survey are shown in Image 1 below. Students recorded their self perceptions using a 4-point Likert scale (1=lowest, 4=highest).
Image 1.
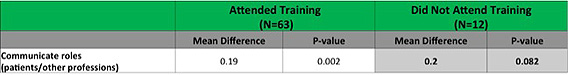
As you can see, the change in perceived competency increased significantly in almost all of the areas measured. In addition, perception of all competencies within the group of pharmacy students alone increased significantly. Regarding the results without significant increases, we completed a further analysis of the data as shown in Images 2 and 3 below.
Image 2.
Image 3.
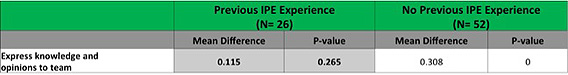

From these analyses, it appears that those who attended training before the events perceived their ability to communicate roles to other patients and professions was increased. This makes sense, as these students participated in icebreakers and were trained in a more intimate setting with a variety of disciplines, instead of their first experience in a team environment being in practice, which we commonly find in our current practice settings. It was also interesting to see that those with previous interprofessional experience did not feel they were better able to express knowledge and opinions to the team, whereas those with no previous interprofessional education did feel this ability increased. This suggests that participation in all interprofessional activities, even if their structures differ significantly, benefits the students in their ability to express their knowledge and use their discipline-specific skills within the team, as our program was a novel approach to interprofessional education for this student population.
So, what does this all mean? How can I incorporate interdisciplinary education into my practice if I’m not faculty within an academic institution like CSU? Fortunately, there are many opportunities to interact with other disciplines outside of the college setting. Collaboration in events such as ours is certainly facilitated more easily when all disciplines are located on the same campus, but they don’t have to be. Are there other schools and disciplines within your institution for which employees precept students? This is an excellent opportunity, if so, as many other disciplines are also moving towards integration of interprofessional education, and in my personal experience I have found that other professions are typically very eager to sign on to collaboration. You also don’t need to only facilitate collaboration among students alone – for example, I am currently working with a physician within my ambulatory practice to conduct a “student exchange,” where my pharmacy students on rotation will work with the physicians at least one day during their time with me, and the attending’s medical students will sign on with me for that day. If you don’t work within a large academic hospital, but you have ties to your local alma mater, or even friends or family who are involved in another health discipline, these may be more great places to start.
When constructing these experiences, I have certainly found one thing to be the most helpful piece overall: don’t be shy! The most important thing to keep in mind is that as hard as we may be searching for opportunity, other disciplines are probably looking too, as the push towards this kind of education is felt within a variety of health disciplines, not just pharmacy alone. Don’t be afraid to reach out to other resources within your site or the community, even if you don’t have close ties; it may be the perfect place for those relationships to start!
College Connections
Indian Health Services: A Unique Pharmacy Rotation in Ambulatory Care
by Vincent Tam, PharmD Candidate 2014, Midwestern University Chicago College of Pharmacy
Compassion, integrity, professionalism and empathy are terms we have heard from the very first day of pharmacy school. Not until I was on rotations did I truly begin to understand the meaning of these words. As a result of the guidance from my mentors, their words of wisdoms, and genuine acts of selflessness with regard to the care of their patients, I am now fully committed to my profession. The experiences I obtained from each rotation have been tremendously beneficial in my growth as a future healthcare professional. One rotation I will describe here is the Indian Health Services (IHS) at Fort Peck in Poplar, Montana. This rotation was unique because not only was I able to practice pharmacy and see the clinician side of the healthcare spectrum, but I was also given the opportunity to learn about the cultural and social aspects of a Native American reservation.
 The IHS pharmacy team led by my preceptor, Dr. Bradley Moran, is an exemplary group of health care professionals. Everyone was kind, a team player, and willing to instruct and assist me whenever I needed. Dr. Moran was readily available as a mentor and showed me the true meaning of pharmacy. By working with Dr. Moran, I was able to see that pharmacists do more than just focus on drugs. Pharmacists at IHS are heavily involved in patient care and they have significant leadership roles, such as leading P&T committees and pain management conferences. When I wasn’t working in the pharmacy, I was helping the clinic providers with their diabetes clinics or attending teleconferences to discuss treatment options for complicated patients with other IHS clinics around the country. We, as pharmacists, are an integral part of the health care system.
The IHS pharmacy team led by my preceptor, Dr. Bradley Moran, is an exemplary group of health care professionals. Everyone was kind, a team player, and willing to instruct and assist me whenever I needed. Dr. Moran was readily available as a mentor and showed me the true meaning of pharmacy. By working with Dr. Moran, I was able to see that pharmacists do more than just focus on drugs. Pharmacists at IHS are heavily involved in patient care and they have significant leadership roles, such as leading P&T committees and pain management conferences. When I wasn’t working in the pharmacy, I was helping the clinic providers with their diabetes clinics or attending teleconferences to discuss treatment options for complicated patients with other IHS clinics around the country. We, as pharmacists, are an integral part of the health care system.
My rotation in Montana was also memorable because of my exposure to the cultural and social aspects of the reservation. My interactions with the Native Americans on a daily basis opened my eyes to the needs of an underserved population. As a population, diabetes is very prevalent and affects people across the age spectrum. There were children as young as two years of age who were on metformin. Lifestyle and dietary choices are huge contributing factors to the many problems evident in this group of people. On top of that, poverty, drug abuse, and lack of medication adherence are all major issues that I came across. Unfortunately, these factors are not so easy to change and knowing this I have come to understand that healthcare is not as black and white as it can sometimes seem. There are many patient-specific underlying issues that must be taken into consideration when caring for patients.
When I wasn’t busy with pharmacy work, I was able to do many interesting and fun activities. I spent the weekends shooting off an assortment of guns, riding four-wheelers, and fishing for dinner. During my exploration of the reservation, I found myself fascinated with the intricacies of Native American crafts like hand woven quilts and the natural beauty of Montana. Jogging through vast open lands and witnessing the vibrancy of the Northern Lights had to be one of the most awe-inspiring experiences of my life.
Overall, my experience during my IHS rotation was extremely positive. I am thankful I had the opportunity to work alongside such great healthcare professionals who strive to make a difference for an underserved population. The folks at the reservation were very welcoming and easy to connect with on a personal level. They never made me feel like an outsider and I really felt like a member of the team. For me, this rotation reinforced the fact that each patient is unique. Being able to connect on a personal level with patients and empower them to be proactive in the management of their diseases is a crucial part of a patient’s therapy. A most valuable lesson that I have learned is that a good healthcare professional is not measured by titles or accolades, but by their willingness to help every patient to the utmost of his or her ability without taking any shortcuts. To be a good healthcare professional, you must be someone who can encourage patients and someone with whom patients can build trust. I want to express my gratitude to my IHS friends and make a promise to them that I will become a pharmacist worthy of the words, compassion, integrity, professionalism and empathy they displayed.
Patient Care Projects to Promote American Pharmacists Month
by Krista Foley PS-3, SSHP Secretary; Lina Hartnett, PS-1, SSHP P-1 Liaison; Ada Acevedo PS-1 SSHP P-1 Liaison, Roosevelt University College of Pharmacy
Roosevelt University College of Pharmacy’s Student Society focuses on enhancing student learning through experiential patient care projects. Our chapter was provided with an opportunity to participate in a health fair event at St. Alexius Corporate Center. Alexian Brothers Medical Center and St. Alexius Medical Center host an annual health fair to inform and educate their employees. During the health fair, employees came in before work, after work, or during a break for point of care cholesterol testing, flu vaccine, blood pressure checks or to determine their weight, body measurements, or calculated body mass index (BMI) using a hi-tech scale. Under the supervision of nurses and nurse practitioners, student pharmacists assisted in checking blood pressures, preparing flu shots, and measuring body composition. Roosevelt University College of Pharmacy prepares its students early through blood pressure education in the first year of the curriculum. First year pharmacy students learn how to check blood pressure utilizing the two-step technique and have the opportunity to master this skill through patient care projects similar to this experience. Body composition measurements, however, was something new to many of our student members.
It was definitely a rewarding experience to see a handful of employees take time out of their busy day to be proactive about their health. As a student pharmacist, this will definitely be an event to remember. With so many health issues arising, it is very important as healthcare professionals to perform preventative care services. It gives the community an idea of where they are at as far as blood pressure and weight, which comprise the two main risk factors that may lead to cardiac-related health problems. In addition, educating the community allows healthcare professionals to point out that both of these risk factors are highly modifiable through life-style modifications such as diet and exercise.
Roosevelt University’s Student Society also participated in a second patient care project as part of American Pharmacists Month. The first-year professional pharmacy students were given the opportunity to represent our organization by coordinating and presenting a seminar about the most common vaccinations indicated in the elderly patient population. Student Society of Health-System Pharmacy student members collaborated with the American Pharmacists Association and the Academy of Managed Care Pharmacy student chapters to develop and deliver the seminar. The seminar was open to the entire Roosevelt community, including the Institute of Continued Learning, and it was delivered by our first and second year pharmacy students. The audience was provided with information regarding influenza, pneumococcal, and herpes zoster vaccines. The audience was provided with Vaccine Information Statements for each of these vaccines as well as a copy of the current recommended immunization schedule for adults. Each student chapter presented basic information on their assigned vaccine and the disease it can help prevent. The specific topics covered during the presentation included signs and symptoms of the disease, minimizing the spread of the disease, available vaccinations for prevention, the current immunization recommendation for adults, and frequently asked questions and myths. Following all three presentations, the audience was given the opportunity to ask questions, which were answered by our Student Pharmacists and Clinical Faculty.
Roosevelt University’s Student Society’s P-1 Liaisons helped to coordinate the influenza presentation from scratch by recruiting a team of first year student members, who were assigned a topic inclusive of one of the following: what is influenza virus, how does it spread, signs and symptoms, complications, available FDA-approved vaccines, or common myths. The presentation was put together by set deadlines and edited by our Chapter Advisor. We were given full responsibility for developing the team and overseeing the creation of the presentation, which gave us a sense of ownership in the presentation as well as helped us develop our leadership skills. We had the opportunity to provide important information to help prevent onset of future viruses and diseases. Presenting to an attentive and actively engaged audience reinforced the impact and need for pharmacist involvement in the community.
These were definitely good experiences for the students of our organization and these patient care projects reiterated the goals of the Student Society of Health-System Pharmacy about promoting interprofessional activities as well as experiential learning.
More
Officers and Board of Directors
TOM WESTERKAMP Immediate Past President224-948-1528 tom_westerkamp@baxter.com
LINDA FRED
President-Elect
217-383-3253 linda.fred@carle.com
GINGER ERTEL Treasurer 660-342-5022 gertel@msn.com CAROL HEUNISCH Secretary 847-933-6811 cheunisch@northshore.orgTRAVIS HUNERDOSSE Director, Educational Affairs Travis_Hunerdosse@rush.edu
JENNIFER ELLISON Director, Marketing AffairsJennifer.C.Ellison@osfhealthcare.org
DESI KOTIS Director, Professional Affairs
JENNIFER PHILLIPS Assistant Editor, KeePosted 630-515-7167 jphillips@midwestern.edu KATHRYN SCHULTZ Regional Director North
JULIE BUCEK Student Chapter LiaisonUniversity of IL C.O.P. bucek@uic.eduNADIYAH CHAUDHARY President, Rockford Student Chapter University of IL C.O.P. nadi925@gmail.comJANEY YU President, Student ChapterMidwestern University C.O.P. janey.yu@mwumail.midwestern.edu
BERNICE MAN President, Student Chapter Chicago State University C.O.P. bman@csu.edu TRAMAINE HARDIMON Student Representative Chicago State University C.O.P thardimo@csu.edu ZAK VINSON President, Student Chapter Southern Illinois University S.O.Pzvinson@siue.edu
ALEX MERSCH President, Student Chapter Roosevelt University C.O.P. amersch@mail.roosevelt.edu
JENNIFER AGUADO President, Student Chapter Rosalind Franklin University C.O.P. jennifer.aguado@my.rfums.org SCOTT MEYERS Executive Vice President, ICHP Office 815-227-9292 scottm@ichpnet.org
ICHP AFFILIATES
PETE ANTONOPOULOS President, Northern IL Society (NISHP) JULIA SCHIMMELPFENNIG President, Metro East Society (MESHP) jschimmelpfen@sebh.org MEGAN METZKE President, Sangamiss Society memiller8@yahoo.com
ED RAINVILLE President, West Central Society (WSHP) 309-655-7331x ed.c.rainville@osfhealthcare.org
Vacant Roles at Affiliates —
Director, Government Affairs; President, Rock Valley Society; Southern IL Society; Sugar Creek Society
Welcome New Members!

New Member Recruiter
Michael Adu-Gyamfi
Michael Augustynowicz
Krishna Bagale
Taylor Barkley
Lillian Bellfi
Brian Bergquist
Khaled Bleibel
Erika Bocklund
Katherine Bullman
Mark Burgess
Ting Chen
Antoinette Cintron
Aristide Cioe
Peter Davito
John Day
Redi Dema
Daniel Dickson
Rubi Doctolero
Roberta Dume
Matthew Fiscella
Jesus Garcia
Vanessa Godek
Adam Hartley
Michael Hildebrandt
Kenya Johnson
Adam Johnson
Theresa Kodua
Akwasi Koduah
Michael Koronkowski
Marica Laketic
Christine Le
Tam Le
Serjo Martinez
Daniel McCarville
Ibrahim Mehdi
William Middleton
Stacie Moltzan
Ruth Nartey
John Nissan
Yaa Nyantakyi
Sam Olson
Jong Park
Viva Pham
Natalie Ravnikar
Shannon Riley
Keith Riley
Cynthia Riley
Nicole Serafin Greg Biedron
Michelle Shalaby
Meghan Shively
Shoaib Siddiqui
Lori Smith
Gina Stassinos
Bridget Sterling
Nila Sturlin
Yen-Nhi Thieu
Kim Thomas
Gelah Villarino
Tramy Vo
Brandon Webb
Kyler Wiegel
Gobena Workneh
Alice Yim
ICHP Pharmacy Action Fund (PAC) Contributors
Names below reflect donations between January 1, 2013 and January 1, 2014. Giving categories reflect each person's cumulative donations since inception.
GENERAL ASSEMBLY GUILD - $1000 & More Scott BergmanKevin ColganEdward DonnellyDave HicksFrank KokaislWilliam McEvoy
Scott Meyers
Michael Novario
Michael Weaver
Trish Wegner
Thomas Westerkamp
SPRINGFIELD SOCIETY - $500-$999 Stephanie CrawfordRauf Dalal
CAPITOL CLUB - $250-$499
Margaret Allen
Vern Johnson
Janette Mark
Edward Rainville
Heidi Sunday
Jill Warszalek
LINCOLN LEAGUE - $100-$249
Anonymous
Marie Williams
GRASSROOTS GANG - $50-$99
Susan Berg
Jennifer Ellison
Tory Gunderson
Glenna Hargreaves
Jerry Storm
CONTRIBUTOR - $1-$49 John Chaney
Izabela Wozniak
Upcoming Events

Tuesday, January 14
CPE Event! Sangamiss Program: Biosimilar Agents: Questions and Controversies Surrounding Their Release
Pao Bistro | Springfield, IL
Tuesday, January 21
Non-CPE NISHP Program: Roles in Helping to Improve Patient Understanding and Accurate Use of Humulin® R U-500 (Concentrated) (regular insulin human injection, USP [rDNA origin])
Seasons 52 |
Oak Brook, IL
Tuesday, January 21 and Wednesday, January 29
CPE LIVE Webinar! Champion Program: Transitions of Care: Project RED at Mount Sinai Hospital
Wednesday, January 29
Pharmacy Directors Network Dinner
Via Carducci | Chicago, IL
Tuesday, February 11
CPE Event! NISHP Program: 8th Annual Leg Day 101: Preparing to be a Pharmacy Advocate
UIC College of Pharmacy | Chicago, IL
Wednesday, March 5
Pharmacy Legislative Day
State Capitol | Springfield, IL
Friday, March 28 - Saturday, March 29
2014 ICHP Spring Meeting: Taking Bold Steps for Patient Care
Marriott Hotel & Conference Center | Bloomington-Normal, IL
_web578x100.png)
Print Entire Issue



 President's Message
President's Message Directly Speaking
Directly Speaking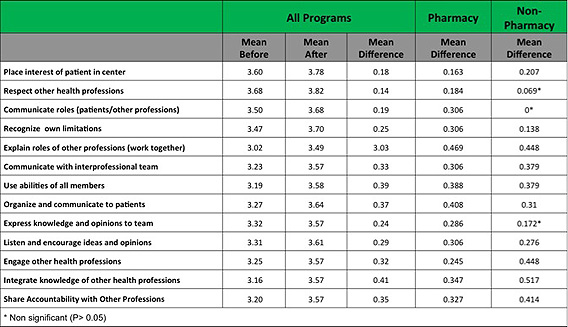

 The IHS pharmacy team led by my preceptor, Dr. Bradley Moran, is an exemplary group of health care professionals. Everyone was kind, a team player, and willing to instruct and assist me whenever I needed. Dr. Moran was readily available as a mentor and showed me the true meaning of pharmacy. By working with Dr. Moran, I was able to see that pharmacists do more than just focus on drugs. Pharmacists at IHS are heavily involved in patient care and they have significant leadership roles, such as leading P&T committees and pain management conferences. When I wasn’t working in the pharmacy, I was helping the clinic providers with their diabetes clinics or attending teleconferences to discuss treatment options for complicated patients with other IHS clinics around the country. We, as pharmacists, are an integral part of the health care system.
The IHS pharmacy team led by my preceptor, Dr. Bradley Moran, is an exemplary group of health care professionals. Everyone was kind, a team player, and willing to instruct and assist me whenever I needed. Dr. Moran was readily available as a mentor and showed me the true meaning of pharmacy. By working with Dr. Moran, I was able to see that pharmacists do more than just focus on drugs. Pharmacists at IHS are heavily involved in patient care and they have significant leadership roles, such as leading P&T committees and pain management conferences. When I wasn’t working in the pharmacy, I was helping the clinic providers with their diabetes clinics or attending teleconferences to discuss treatment options for complicated patients with other IHS clinics around the country. We, as pharmacists, are an integral part of the health care system.




_web578x100.png)